Hearing the words “herniated disc” can be frightening.
Many patients immediately imagine surgery, long-term pain, or not being able to live normally again.
And almost immediately, the same questions come up:
- “Do I need surgery?”
- “Can this get better naturally?”
These are some of the most common questions I hear in an orthopedic clinic.
The short answer is this:
● Yes — in many cases, a herniated disc can improve naturally without surgery.
What Is a Herniated Disc?
A herniated disc occurs when the soft inner portion of the spinal disc pushes out beyond its normal boundary.
This disc material can irritate nearby nerves, leading to symptoms such as:
- Lower back pain
- Pain radiating to the buttock or leg (sciatica)
- Numbness or tingling
- Occasionally, weakness in the leg
Herniated discs are most common in the lumbar spine because this area bears the greatest mechanical stress during daily activities.
Can a Herniated Disc Really Heal Naturally?
Yes — in selected cases, it can.
Natural improvement is more likely when:
- Pain gradually decreases over time
- There is no progressive muscle weakness
- Daily activities remain mostly possible
- The disc herniation is mild to moderate
In real clinical practice, I see many patients whose symptoms gradually improve
even though the MRI findings remain unchanged for some time.
Over time — often within several months, and sometimes up to 1–2 years — the body may respond by:
- Reducing inflammation around the nerve
- Gradually shrinking or reabsorbing the herniated disc material
This process is known as spontaneous disc resorption, and it has been well documented in medical imaging studies.
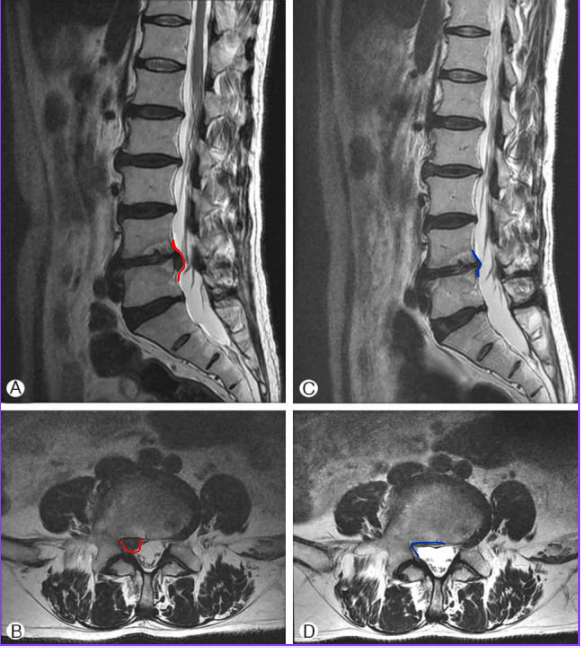
Source: National Institutes of Health (NIH), Open-i
Does That Mean Everyone Should Just Wait?
Not necessarily.
Natural healing is not appropriate for every patient.
More active treatment — and sometimes surgery — may be required if:
- Pain continues to worsen
- Leg weakness develops
- Numbness progresses
- Bowel or bladder dysfunction appears (this is a medical emergency and requires immediate evaluation)
- Symptoms persist despite months of conservative treatment
In these situations, delaying care may increase the risk of permanent nerve damage.
What Matters While Waiting for Natural Recovery
Choosing conservative treatment does not mean doing nothing.
Proper management usually includes:
- Pain control with medication or injections
- Activity modification to reduce spinal stress
- Avoiding deep forward bending or prolonged floor sitting
- Light activity such as walking, as tolerated
During the acute pain phase, aggressive stretching or improper exercise can actually worsen symptoms.
A personalized rehabilitation plan is often more important than simply “resting.”
A Final message from the clinic
A herniated disc can improve naturally —
but not every disc should be treated the same way.
MRI findings alone do not determine whether surgery is needed.
The most important factors are:
- Your symptoms
- How those symptoms change over time
- How much they affect daily life
What matters most is not the MRI image itself, but how your symptoms evolve over time. Treatment decisions should always be guided by your daily function and neurological findings.
For a broader understanding of back pain and how disc problems fit into the overall picture, see our overview of back pain.
Leave a Reply