A Patient-Friendly Guide to Ultrasound vs X-ray vs MRI
In orthopedic outpatient clinics, ultrasound is used very frequently.
Among orthopedic specialists, ultrasound has become increasingly important and versatile—so much so that it is often described as the orthopedic equivalent of a stethoscope in internal medicine.
When patients are advised to undergo an ultrasound exam, these questions commonly arise:
“Can’t I just choose either MRI or ultrasound?”
“I’ve heard ultrasound isn’t very accurate.”
“If my X-ray is normal, why do I still need an ultrasound?”
In reality, orthopedic ultrasound can be more useful than MRI in certain clinical situations.
In this article, we’ll explain:
- When and why ultrasound is used in orthopedics
- How ultrasound differs from X-ray and MRI
- How doctors choose the most appropriate imaging test
from a patient’s perspective.
What Is an Orthopedic Ultrasound Exam?
Ultrasound imaging uses high-frequency sound waves that are transmitted into the body.
The images are created based on how these sound waves are reflected back from different tissues.
This allows physicians to visualize and differentiate structures in real time, including:
- Muscles
- Tendons
- Ligaments
- Nerves
- Structures surrounding joints
Key advantages of ultrasound include:
✔ No radiation exposure
✔ Short examination time
✔ Ability to examine structures while the patient is moving
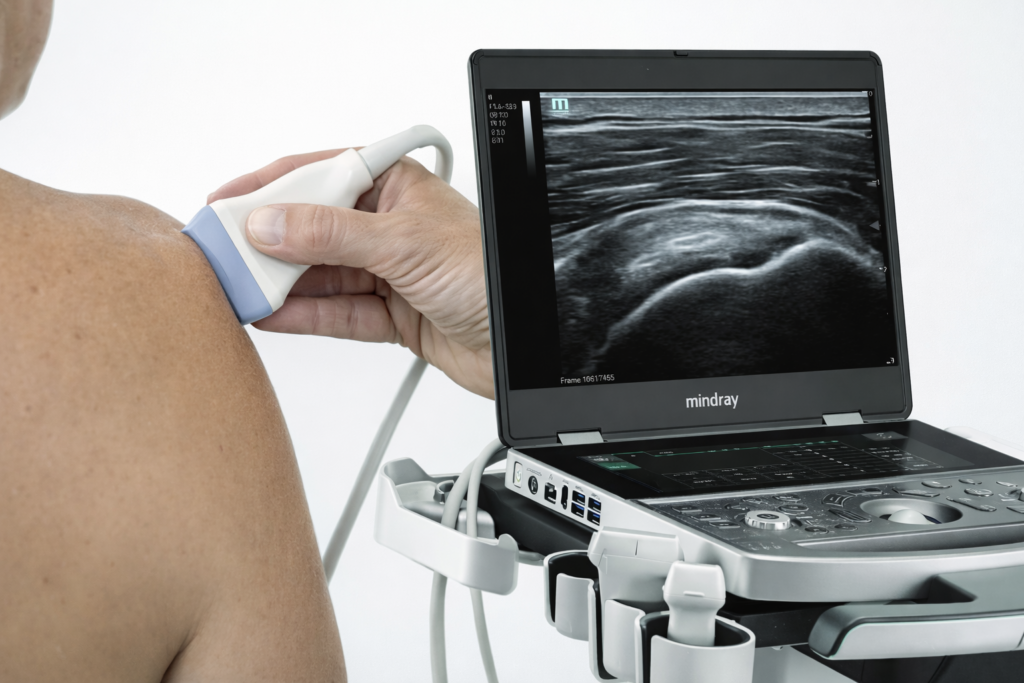
What Structures Are Best Evaluated with Ultrasound?
Ultrasound is particularly effective for evaluating soft tissues, such as:
- Tendons (e.g., rotator cuff, Achilles tendon)
- Ligaments
- Muscles
- Joint effusion (fluid inside a joint)
- Cysts or hematomas (fluid-filled collections)
- Peripheral nerves
However, ultrasound has limitations when it comes to:
- Internal bone structures
- Deep joint components
Common Clinical Uses of Ultrasound in Orthopedics
1. Suspected Tendon or Ligament Injury
Examples include:
- Shoulder pain (rotator cuff disorders)
- Ankle sprains (ligament injuries)
- Tennis elbow or golfer’s elbow (tendinopathy)
In many of these cases, X-rays appear normal because they primarily show bone.
Ultrasound allows doctors to directly assess tendon and ligament damage or inflammation at the point of care.
2. Evaluating Pain During Movement
One of ultrasound’s greatest strengths is its ability to provide dynamic, real-time assessment.
This means the physician can examine the affected area while the patient moves, which is especially helpful when:
- A joint produces clicking or snapping sounds
- Pain occurs only during certain movements
- A tendon appears to “catch” or shift abnormally
In these scenarios, ultrasound can sometimes provide more clinically relevant information than MRI.
3. Detecting Joint Fluid, Cysts, or Hematomas
Ultrasound is commonly used to assess:
- Knee joint effusion
- Wrist or finger ganglion cysts
It enables physicians to quickly locate fluid collections, and if necessary, aspiration or drainage can be performed under ultrasound guidance during the same visit.
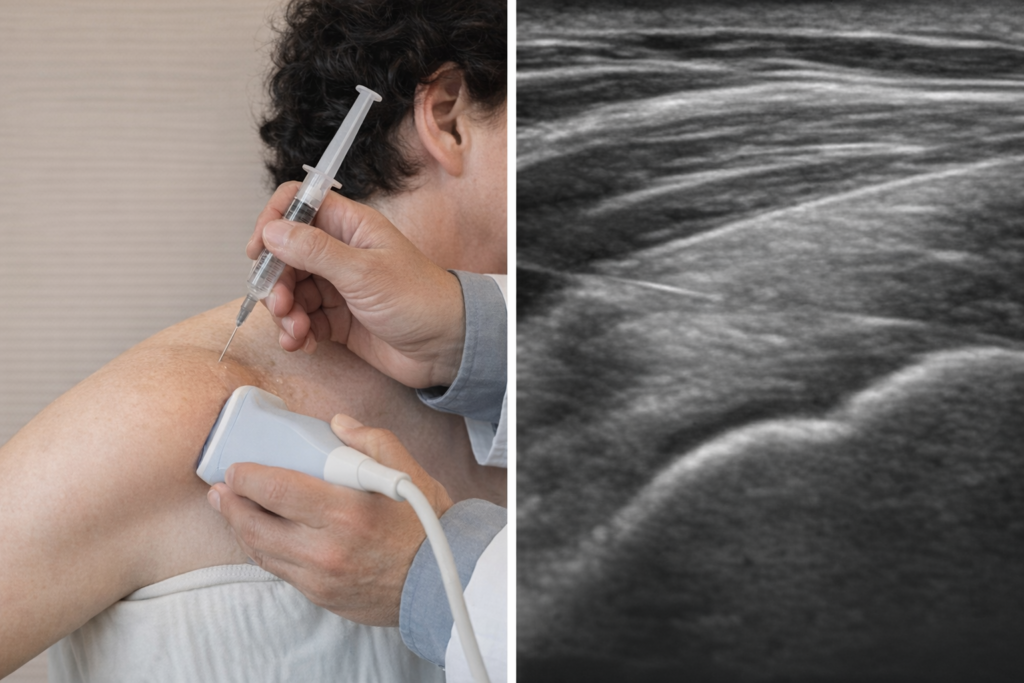
4. Improving Accuracy and Safety of Injections
Orthopedic ultrasound truly shows its value when combined with image-guided injections, such as:
- Intra-articular joint injections
- Peritendinous injections
- Perineural or ligament-adjacent injections
Ultrasound-guided injections allow the physician to:
- Deliver medication precisely to the target area
- Avoid nearby nerves, vessels, and tendons
- Improve treatment effectiveness and safety
The shoulder is the most commonly treated joint, but ultrasound-guided injections are also widely used for the hand, foot, hip, and spine.
5. When MRI Is Not Immediately Ideal
Ultrasound can be an excellent initial option when:
- Symptoms are mild or in an early stage
- MRI is physically difficult for elderly patients
- MRI wait times are long
- Cost is a concern
In these cases, physicians often start with ultrasound, treat based on findings, and reserve MRI for situations where symptoms persist or worsen.
This stepwise approach is commonly used in real-world orthopedic practice.
Can Ultrasound Replace MRI?
Not in every situation.
Ultrasound has limitations in evaluating:
- Deep joint structures
- Internal cartilage or disc pathology
- Global assessment of complex joints
MRI remains particularly valuable when:
- Surgical planning is required
- Deep soft tissue pathology is suspected
- The extent of tendon tears or muscle degeneration must be fully assessed
How Do Doctors Choose Between X-ray, Ultrasound, and MRI?
A simplified comparison:
- X-ray → Bones, fractures, dislocations, joint alignment
- Ultrasound → Tendons, ligaments, nerves, fluid, real-time movement
- MRI → Deep soft tissues, cartilage, comprehensive joint evaluation
The choice of imaging depends on symptoms, physical examination findings, and clinical judgment.
A Final Message From the Clinic
Ultrasound is not an inferior version of MRI.
It is a different tool designed for a different purpose.
When used appropriately, orthopedic ultrasound is:
- Fast
- Safe
- Clinically accurate
If you’re unsure which imaging test is right for you, discussing your symptoms and concerns with your physician will help determine the most appropriate and effective evaluation.
We hope this guide helps clarify how imaging choices are made in orthopedic care.
This article is part of a series explaining how imaging tests are used in orthopedic care.
For a complete overview of imaging tests in orthopedic care, please refer to:
👉 X-ray, CT, MRI, and Ultrasound: What’s the Difference and Why Are There So Many Tests?
Leave a Reply